Optical coherence tomography (OCT) technology utilization in the management of posterior segment diseases has increased significantly in the past decade. But often, as with any technology, we are likely to find the imaging protocols that work best for us ourselves. Gradually over time, we tend to use the same testing strategies over and over again. One of the main advantages of today’s OCT platforms is that many different imaging systems and analyses are available so that each practitioner can build the exact platform to suit their own clinical needs.
For example, OCT software modules can be incredibly valuable in determining the stability of glaucoma. OCT angiography is valuable in determining the presence or absence of subretinal neovascularization. Multimodal imaging can highlight various layers of the retina, which is important in the management of diseases such as diabetic retinopathy, as the “middle” layers of the retina are mainly affected. As discussed previously, fundus autofluorescence (FAF) is important in managing geographic atrophy (GA).
I had a patient just this week who was in for a glaucoma follow-up complaining of blurry vision. This pleasant 97-year-old woman also has a history of a pituitary adenoma partially resected about 12 years ago, following her similar complaints of decreased vision after cataract surgery. The neuroimaging I had ordered at that time demonstrated a rather large adenoma invading the left cavernous sinus. Fortunately, this has remained stable since resection. But with her being 97 years old, you would expect some macular changes also to be in play—and you would be correct. She did have early GA, which ultimately was the basis for her progressed complaints of decreased vision. Did I mention she also has primary open-angle glaucoma (POAG)?
There has been much talk lately on the topic of GA, especially now that there are viable treatment options to slow down the progression of the disease. FAF plays a crucial role in showing the areas of retinal pigment epithelium (RPE) that have already atrophied. But more importantly, FAF can highlight the areas of the RPE that will atrophy—and this is important in determining who is best suited for these new GA treatments so that they can be initiated earlier in the disease process.
Geographic atrophy often starts in the perifoveal region and over time expands centrally and toward the outer aspects of the macula. Oftentimes in the early stages of the disease, as the RPE sub fovea is unaffected, vision is also relatively unaffected. However, as the foveal RPE begins to atrophy, vision also begins to decline.
Figure 1 is a Spectralis (Heidelberg Engineering) OCT scan of this 97-year-old woman showing classic findings associated with GA: RPE disruption and concurrent disruption of the overlying outer retinal anatomy. This is how we typically evaluate the retina in patients with macular degeneration. As mentioned, FAF plays a role in identifying where the next areas of the retina are likely to suffer the effects of this progressive disease.
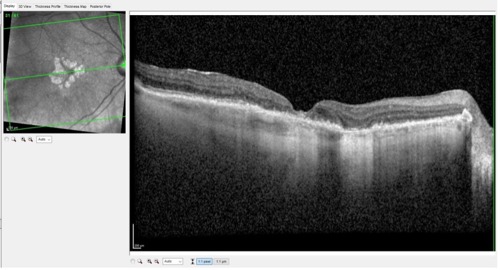
As with our practice management software, most of us use only a portion of what the specific software can accomplish. Likewise, our OCT instruments have the capability of doing far more than what we tend to gravitate toward using on a daily basis.
By simply reversing the black-and-white image of our en face view, we can get a much better picture of the extent to which the RPE has been affected. In other words, doing so gives us a 10,000-foot view of the damage to the RPE. This in turn enables us to get a better clinical feel for the expanse and depth of the RPE atrophy and, consequently, the expected visual acuity.
Figures 2, 3, and 4 below show the fellow eye of this patient over a 2-year period using the method described above. By simply reversing the black-and-white image, the lack of RPE tissue appears as a “hole” in the retinal tissue. A smaller hole well outside the fovea would have little impact on vision, whereas a larger hole centered in the fovea would have a much more significant impact on vision.
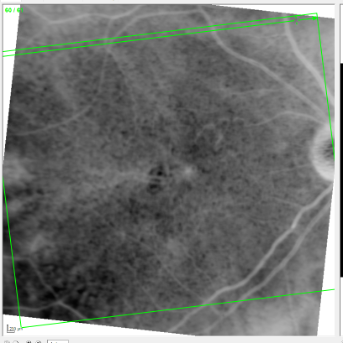
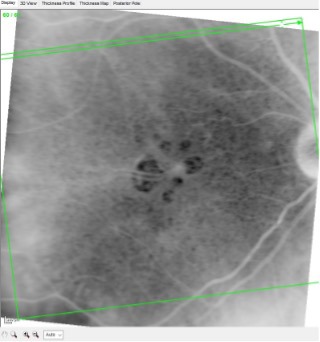
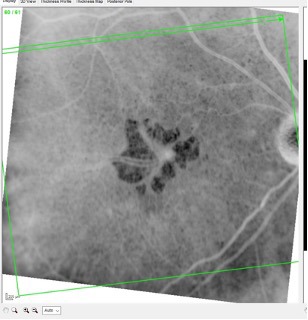
In Figure 4, note the “holes” in the RPE that I mentioned earlier and the extent to which the fovea is involved. The large vessels seen centrally are subfoveal choroidal vessels, and they readily shine through the area lacking RPE tissue. Needless to say, this would significantly affect visual acuity—and it does, which is the basis of her complaints.
Sometimes looking at the same picture in a different way gives an entirely different perspective. Use your OCT technology to its fullest capabilities; you may be surprised at how helpful it is.
This editorial content was supported via unrestricted sponsorship




