A 68-year-old African American male presented with symptoms of blurry vision bilaterally without glasses. He denied distortions or floaters in either eye. His ocular and medical history were unremarkable. Entrance testing showed normal range of motion, full to finger counting, and normal pupillary response. His BCVA measured 20/20 OD and OS. Slit lamp biomicroscopy revealed grade 1 nuclear sclerosis OU. Intraocular pressure was 13 mm Hg OD and 13 mm Hg OS. Dilation revealed bilateral posterior vitreous detachments with Weiss ring.
His optic nerves were flat, sharp with good color, and measured 0.50 H/V bilaterally. The retinal blood vessels were well perfused and of normal caliber. The macula was mottled with small, central drusen OS. The right macula had multiple drusenoid pigment epithelial detachments with intermediate drusen. There was also evidence of a “double-layer” sign, suggesting a flat occult choroidal neovascular membrane. Multimodal imaging including OCT and OCT angiography (OCTA) were obtained to further evaluate for the presence of exudation or leakage.
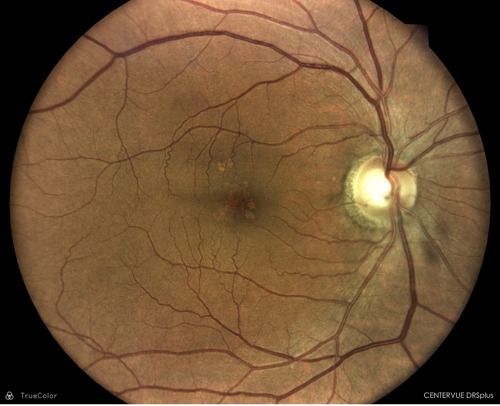
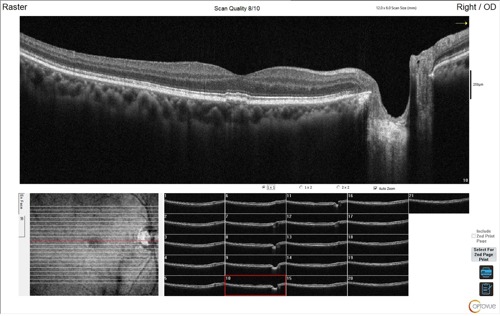

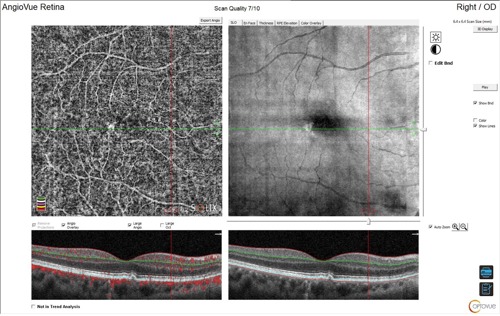
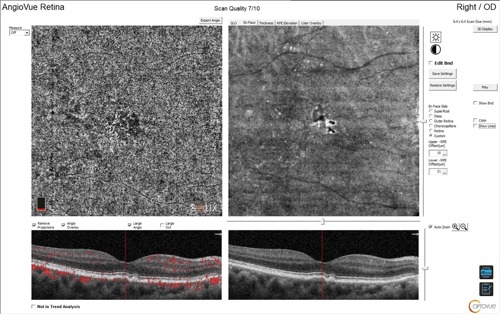
- No visible leakage or exudation
- En-face OCTA choriocapillaris slab shows a macular neovascular complex
- Corresponding structural OCT with flow overlay demonstrates flow underneath the retinal pigment epithelium and above Bruch’s membrane
This patient was diagnosed with a nonexudative occult neovascular membrane (ie, macular neovascularization). These lesions do not show active exudation or leakage. Close analysis with OCTA will highlight increased flow in that area with a neovascular frond in the choriocapillaris slab. He was referred to the retina specialist for further evaluation.
Clinical Pearls:
- OCTA advances patient care in nonexudative AMD by improving understanding of the pathogenesis of the disease.
- Enhanced detection and monitoring of this condition is necessary to watch for progression to exudative disease.
This editorial content was supported via unrestricted sponsorship